
Dupuytren’s Disease
Regain Control Over Your Hands: Your options for Dupuytren’s Contracture
Do you have permanently-flexed fingers that are impacting your daily life? It may be that you’re suffering from Dupuytren’s Contracture.
If this is you, read on to find out about some of the treatment options available to you.
Dupuytren’s contracture, a condition leading to the permanent flexing of one or more fingers, can significantly impact your daily life and activities.
Known by various names such as Dupuytren’s disease, Viking disease, and Celtic hand, it represents a fibromatosis disorder affecting the palms. Dr Gavin Nimon at Glenelg Orthopaedics specialises in treating this condition, offering expert care and options to restore functionality to your hands. If you or a loved one are navigating the challenges of Dupuytren’s contracture, reach out to discover how we can help you reclaim the full use of your hands.
What is Dupuytren’s Disease / Contracture
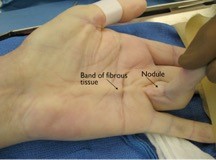
Dupuytren’s Contracture is a hand deformity that usually develops slowly, over decades, but in some people can come on very quickly. It affects the connective tissue under the skin of your palm. It typically starts on the palm of the hand with a small nodule, or several nodules, that can be felt and are initially not very hard. The knots of tissue eventually form a thick cord that can pull one or more of your fingers into a bent position.
Once this occurs, the fingers affected by Dupuytren’s disease cannot be straightened completely, which can affect everyday activities such as placing your hands in your pockets, putting on gloves or shaking hands. It most commonly affects the ring and little fingers
Risk Factors:
The exact trigger that causes the palmar fascia to thicken and contract is unknown. However, contributing factors may include:
- Age – The condition is more common in middle to later years of life, usually starting around middle age.
- Gender – Men are disproportionately affected, with about 10 times more men than women experiencing this condition.
- Heredity – Dupuytren contracture often runs in families, indicating a strong genetic component.
- Ancestry – Those of Celtic or Scandinavian ancestry are particularly at increased risk. This factor is notably significant, as it is most common in people whose families come from these regions.
- Certain medical conditions – Individuals with diabetes not only have a higher risk of developing Dupuytren contracture but also face a greater risk of infection following surgical interventions related to the condition.
Understanding these risk factors can help in early identification and management of Dupuytren contracture. Awareness is particularly important for those who may be at greater risk due to their family history or ethnic background, enabling them to seek medical advice and intervention sooner.
Treatment at Glenelg Orthopaedics:
Treatment depends upon the severity of the condition. In its earlier stages, reassurance is best, as not all cases of Dupuytren’s progress at the same rate.
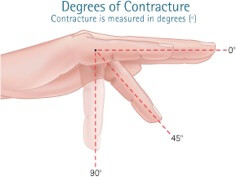
When the condition progresses such that the person is unable to lay their hand palm-down on a flat surface, or their fingers have contracted into their palm so that the hand has functional issues. In these cases Dr Nimon will offer surgery.
During surgery, under an anaesthetic, Dr Nimon makes an incision in the hand to remove the thickened tissue, which can significantly improve the mobility of the fingers. However, some patients may experience a return of contractures and might require subsequent surgeries.
Each treatment option has its benefits and complications, and Dr Nimon will advise you on the benefits of each in your situation.
Next Steps
If you’d like to discuss your specific treatment options might be, contact us to find out what your options are.
